Autonomic Nervous System
The autonomic nervous system is is an involuntary nervous system which is responsible for the minute to minute as well as the day to day functions of the body systems. It is activated mainly by centers in the hypothalamus, brain stem and spinal cord but is influenced to some extent by the cerebral cortex.
Sensory signals from the viscera travel to the spinal cord, brain stem and hypothalamus, and appropriate responses are returned to the viscera. This pathway is called a visceral reflex.
In the sympathetic chain there is an intermediary step between the viscera and spinal cord – a “halfway house” if you will, that runs alongside the spinal cord, and it is called the sympathetic chain. There is therefore a neuron that carries the signal from the spinal cord to the sympathetic chain called the preganglionic neuron, and one that carries the the signal between the ganglion of the chain to the organ called the post ganglionic neuron. The preganglionic fiber is short and the post ganglionic fiber is long.
In general the sympathetic nerves of T1 go to head, T2- T6 to the thorax and T7 -T11 to the abdomen. The nerves of T12 , L1 and L2 go to the legs. This distribution is an approximation and there is a large cross over of geographic coverage from person to person. The innervation in large part is governed by the embryological origin of the tissues. Since the heart for example had its origins in the neck of the developing fetus, sympathetic innervation is from the neck segments. Similalrly the foregut organs arose from the chest endoderm/mesoderm tissues, and so innervation is from the lower thoracic region.
The parasympathetic system is designed differently. It executes its function through the cranial nerves and through sacral segments. Most of its function however is executed through the vagus nerve which covers both the chest and abdominal cavities. It also has a system of preganglionic and post ganglionic fibers, but the preganglionic fibers usually pass into or close to the organ and post ganglionic fibers are dominantly within the organ. Therefore unlike the sympathetic system, the preganglionic fiber is long and the post ganglionic fiber is short.
Within the gastrointestinal tract, the parasympathetic system accelerates digestion by increasing peristalsis and opening valves and sphincters, and increasing blood flow to the digestive organs. In essence it promotes digestion and absorption, which is best done while the person is resting. The sympathetic system is the “fight or flight” component, and directs energy and blood to skeletal muscle and other organs that need energy when a person is active, and in turn directs energies away from the gastrointestinal tract. Thus in the digestive system, it slows things down by slowing peristalsis, closing valves and sphincters, and decreasing blood flow to the digestive tract.
The nerves for the gallbladder run with the cystic artery so that they travel with the celiac axis, and then right hepatic artery and finally with the branches to the gallbladder.
Parasympathetic System
The function of the parasympathetic system with regard to the gallbladder and biliary system is to accelerate the production and delivery of bile to the duodenum so contraction of smooth muscle in the gallbladder is facilitated while the sphincter of Oddi relaxes soas to open the juice gates. The vagus nerve is the parasympathetic component and it arises from both vagal trunks via anterior and posterior trunks. The anterior trunk (left vagus) is connected to the hepatic plexus and is the major supply to the gallbladder. The posterior trunk (right vagus) utilises the celiac plexus and controls the sphincter of Oddi .
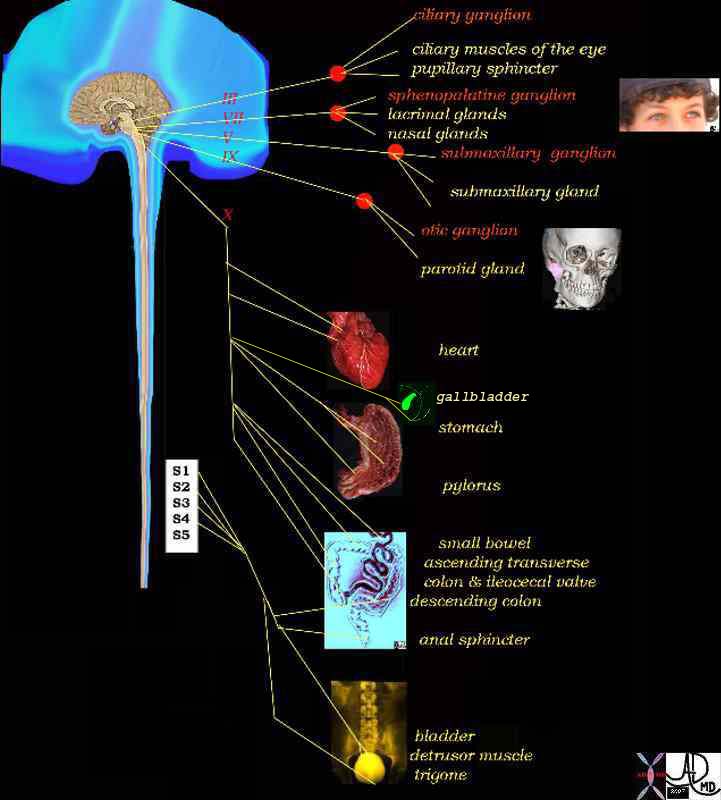
Parasympathetic System |
| The vagus is the parasympathetic nerve that innervates the gallbladder and it has two trunks. The anterior trunk innervates the gallbladder smooth muscle and the posterior trunk that innervates the sphincter of Oddi. The diagram shows the vagus (cranial nerve X) and the extent of its parasympathetic innervation.
14798d08 brain control parasympathetic nervous system ciliary ganglion eyes ciliary muscle pupillary sphincter sphenopalatine ganglion lactrimal glands nasal glands submaxillary glands submaxillary ganglion otic ganglion parotid gland heart cardiac stomach pylorus gallbladder small bowel colon anal sphincter bladder detrusor muscle trigone S1 S2 S3 S4 vagus nerve cranial nerves III oculomotor VII facial nerve V mandibular nerve IX glossophayngeal nerve control efferent system parasympathetic supply Davidoff Art Davidoff MD copyright 2008 |
Applied Biology
Injury or surgical vagotomy to the anterior trunk will reduce gallbladder contractility, promote stasis and predispose to cholelithiasis.
Sympathetic System
The function of the sympathetic system is to slow digestion and hence it inhibits gallbladder emptying by increasing the tone of sphincter of Oddi (hepatopancreatic sphincter ) and by stimulating the release of vasoactive intestinal polypetptide (VIP) at nerve terminals to inhibit gallbladder contraction.
Sympathetic fibers arise from celiac plexus. They travel with the cystic artery. The sympathetic innervation comes chiefly from T2-T10 reaches the celiac ganglia via splanchnic nerves.
The greater splanchnic nerves for the biliary system receives sympathetic supply from T7-9 and the lesser splanchnic nerves from T10 and T11 while the least enters the cord at T12. The celiac plexus transmits afferent fibers from the foregut organs including the gallbladder reaching the spinal cord through the greater splanchnic nerve and via the thoracic sympathetic chain.
Sympathetic fibers originate in the intermediolateral corneal cells in the spinal cord. They traverse out of the spinal column and can travel up, down, or in the region where they exit. These nerves provide the efferent innervation. The afferent signals travel back, much along the same route, but enter the spinal cord through the posterior spinal nerve roots. This afferent/efferent communication is the key to proper muscle contractions.
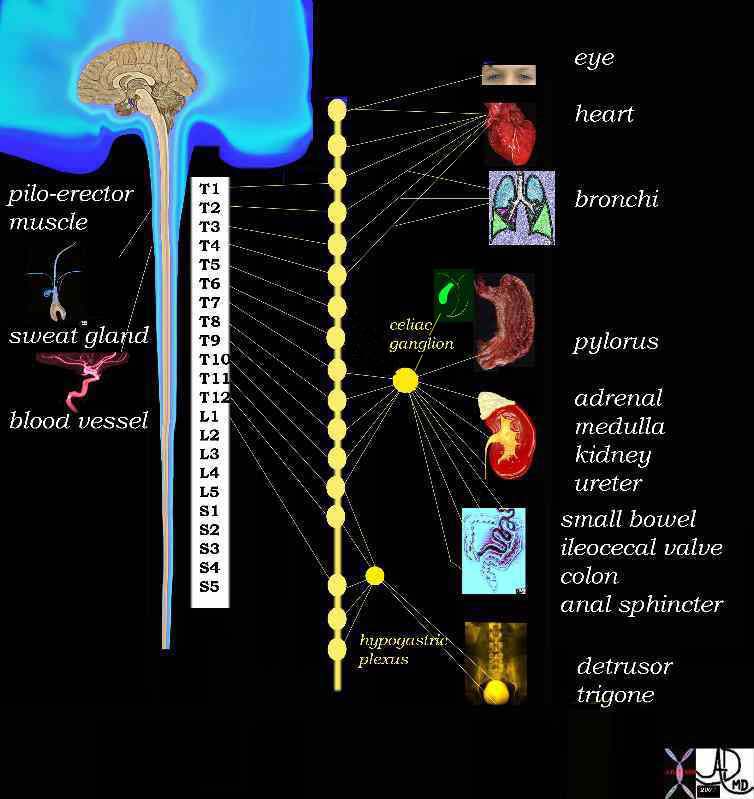
Sympathetic System |
|
From the spinal cord the sympathetic neurons travel to the sympathetic chain that lies along the spinal cord (line of “yellow buttons”. This chain is an intermediary step between the viscera and spinal cord – a “halfway house” There is therefore a neuron that carries the signal from the spinal cord to the sympathetic chain called the preganglionic neuron, and one that carries the the signal between the ganglion of the chain to the organ called the post ganglionic neuron In general T1 goes to head, T2- T6 the thorax and T7 -T11 the abdomen. T12 , L1 and L2 go to the legs. This is an approximation and there is a large cross over. The innervation depends on the embryological origin. Since the heart originated in the neck of the fetus the innervation for the heart is from the cervical sements. Similalrly the foregut organs arise from the chest endoderm/mesoderm and so innervation is from the lower thoracic region . Davidoff Art Davidoff MD 14798d05.800 |
Somatic Nerves
The somatic nerves of the gallbladder are from intercostal nerves T8, T9, and T10 spinal segments which supply the parietal peritoneum. The phrenic nerve is formed from C2,3,4 and 5 supplying the diaphragm, underlying peritoneum, and gallbladder.
Applied Biology
Pain arising from the gallbladder or surrounding peritoneum can be carried by the sympathetic afferent fibers or by the somatic fibers, and will be felt in the corresponding somatomes or dermatomes. Thus pain from the gallbladder is most commonly felt in the right upper quadrant but may be felt in the epigastric area, right shoulder or anterior chest.
-
Afdhal Nezam Gallbladder and Biliary Diseases Published by Informa Health Care, 2000
-
Krishnamurphy Nuclear Hepatology: A Textbook of Hepatobiliary Diseases By G. Krishnamurthy, Shakuntala Krishnamurthy Published by Springer, 2000
- Moore Clinically Oriented Anatomy By Keith L. Moore, Arthur F. Dalley, A. M. R. Agur Published by Lippincott Williams & Wilkins, 2006
